CBS News Live
CBS News Boston: Local News, Weather & More
CBS News Boston is your streaming home for breaking news, weather, traffic and sports for the Boston area and beyond. Watch 24/7.
Watch CBS News

The Patriots are hoping that they have their new franchise quarterback in Drake Maye.

In his new role as an NFL Draft analyst, former Patriots head coach Bill Belichick wasted no time critiquing his old team's new quarterback, Drake Maye.

The Patriots got their quarterback in the first round of the 2024 NFL Draft on Thursday night, but New England's work is far from done this weekend.

College students want their schools to divest from Israel. So how is tuition money linked to the war in Gaza?

Northeastern University is the latest college campus in Massachusetts to see pro-Palestinian student protests.

The alley off Boylston Street in Boston that was full of Emerson College student demonstrators for days now sits empty.

Businesses in Provincetown are running into trouble when to comes to hiring summer employees.

The judge heard arguments on several key motions in the Karen Read murder case ahead of opening statements.

There are plenty of fun and exciting events this weekend to celebrate Spring and the end of April!

A look at the timeline of events in Karen Read's high-profile murder trial.

Aidan Kearney, the blogger known as "Turtleboy," is a key figure in the Karen Read trial.

Karen Read is charged with killing her boyfriend, Boston police officer John O'Keefe.

Lionel Messi will make his first visit to Gillette Stadium on Saturday night, which is a busy one for the Boston sports scene. MLS analyst Taylor Twellman joins WBZ's Dan Roche to discuss the experience of seeing Messi in person, his impact on Major League Soccer, and what makes him such a special competitor.

Jason Mikell has your latest weather forecast.

Police moved in on the pro-Palestinian encampment at Northeastern on Thursday but left after 30 minutes. No arrests were made. Breana Pitts has Friday's top stories.

There are plenty of fun and exciting events this weekend to celebrate Spring and the end of April!
Jason Mikell has your latest weather forecast.

A Townsend woman was scammed into believing a famous actor was in love with her. Then the case took on a potentially more sinister turn.

State contracts obtained by the I-Team show taxpayers are paying tens of millions of dollars to hotels for rooms and food.
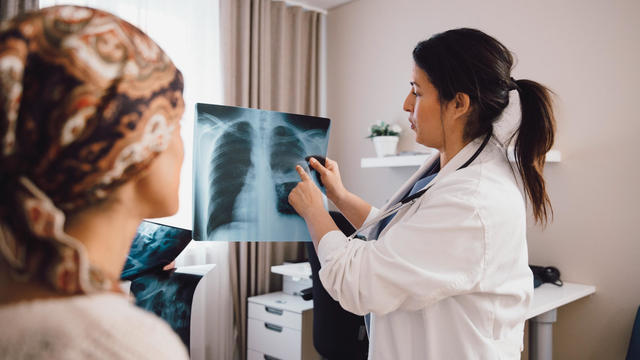
A new study finds that people with breast cancer are more likely to develop a second cancer over time.

The CDC is keeping a close eye on the impact that rising heat is having on o

Was the Drake Maye pick a HIT or a MISS? Are the Patriots WINNERS or LOSERS? Has the franchise found its QUARTERBACK OF THE FUTURE or are the Patriots DOOMED FOR ETERNITY?

"Messi Madness" is set to fully engulf Foxboro this weekend with a crowd of 65,000 expected to head to Gillette Stadium for their chance to see soccer royalty.

The Patriots got their quarterback in the first round of the 2024 NFL Draft on Thursday night, but New England's work is far from done this weekend.

Michael Hurley says the New England Patriots made the right pick with Drake Maye at number 3.

In his new role as an NFL Draft analyst, former Patriots head coach Bill Belichick wasted no time critiquing his old team's new quarterback, Drake Maye.

Drake Maye was rather excited when he sat down for a virtual meeting with Patriots reporters on Thursday night. And that's putting it mildly.

The Patriots are hoping that they have their new franchise quarterback in Drake Maye, whom they drafted third overall Thursday night at the 2024 NFL Draft.

Sitting at No. 3 overall behind two quarterback-needy teams, the New England Patriots didn't really have the benefit of first choice when their time came to make their pick. But that's something they were comfortable with.

With the third overall pick in the 2024 NFL Draft, the New England Patriots selected quarterback Drake Maye out of UNC.

Believe it or not, according to data from the Tax Foundation, Massachusetts ranks better than 13 other states.

When WBZ-TV showed Boston Red Sox fans pictures of current players, few could name any of them.
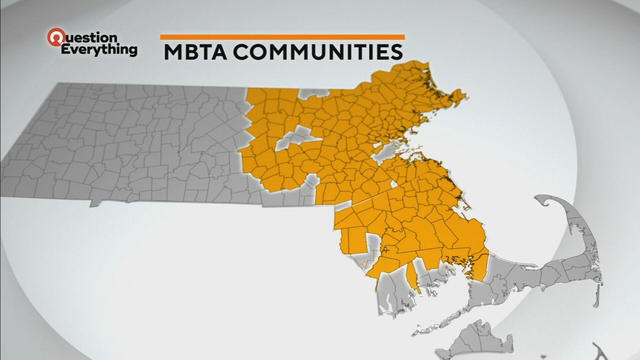
A law designed to ease the housing crunch in Massachusetts is turning into a battle between the state and some communities.

In Falmouth, just down the road from the ferry that heads to Martha's Vineyard, is an aquarium that happens to be a piece of history on Cape Cod.

Ice cream lovers are coming from all over to Holy Cow Ice Cream Cafe for their homemade ice cream and unique flavors.

A Somerville business is bringing pinball players together as they get their nostalgia fix.

A new study finds that people with breast cancer are more likely to develop a second cancer over time.

The CDC is keeping a close eye on the impact that rising heat is having on o
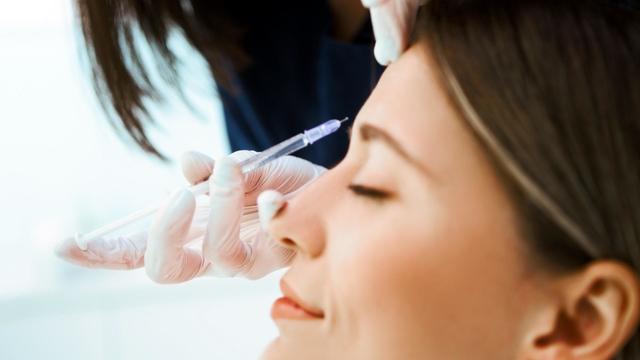
The CDC has issued an advisory about the risks of safely injecting Botox after some people have gotten so sick they had to be hospitalized.

Federal officials say they're double checking whether pasteurization has eradicated the danger from possible bird virus particles in milk.

Members of Gen-Z believe they are aging faster than other generations, but is that true?

A Townsend woman was scammed into believing a famous actor was in love with her. Then the case took on a potentially more sinister turn.

State contracts obtained by the I-Team show taxpayers are paying tens of millions of dollars to hotels for rooms and food.

A fourth-grade teacher at an elementary school in Cambridge is facing child rape charges.

William Foley Jr., a five-time drunk driver who lost his license after a fatal crash in 2001, is back behind bars after an I-Team investigation.

The IRS Criminal Investigation unit helps go after violent criminals, including some right here in Boston.

Quincy City Council President Ian Cain and Swansea attorney John Deaton are seeking the Republican nomination to run against Sen. Elizabeth Warren.

Pro-Palestinian students have accelerated their protests of the Israel-Hamas war. But are the they helping or hurting their cause?

Massachusetts State Sen. Peter Durant weighed in on budget concerns in Massachusetts.

According to ADL's annual Audit of Antisemitic Incidents, Massachusetts had the fifth most incidents in the country last year, up a shocking 189 percent over 2022.

"It's the golden goose," said Rooney of Boston's commercial property taxes, which provides a large percentage of the city's annual revenue.

April 20, 2024 is Record Store Day. See which record shops in Massachusetts are participating.

Boston Dynamics' latest robot is ready to "exceed human capabilities," the company says.

Rising costs are forcing small businesses located on Boston's Massachusetts Avenue to close.

Boston-based box wine brand Alileo teamed up with Caffe Nero to launch a coffee and wine experience in Massachusetts.

Today is Patriots' Day in Massachusetts. Here's what to know about the celebrations and what's open and closed for the holiday.

Researchers spotted a 37-year-old right whale mother named Wolf and her calf off the coast of Massachusetts.

The 2024 cicada broods will not be emerging in Massachusetts - but the buzzing bugs are set to appear here in 2025.

A pair of vultures thought to be "actively dying" actually had too much to drink, wildlife rescuers in Connecticut say.

A fluffy pile of golden retrievers took over the Boston Common in memory of Spencer the marathon dog.

The thick fog made for an eerie sight as the Mayflower II crossed the Cape Cod Canal.

Robert Shure is the talented sculptor behind the FAO Schwartz teddy bear, the Cy Young memorial and the Massachusetts Fallen Firefighters Memorial.

Ming Tsai demonstrates how to cook a traditional Chinese street food - Ming's bings.

Founded out of love, Rustic Marlin is a home décor and lifestyle brand with a unique origin story in Massachusetts.

The Vermont Country Store has since become an iconic destination for locals and tourists alike.

Creating an inviting environment for the community to meet, enjoy and participate in the arts

There are plenty of fun and exciting events this weekend to celebrate Spring and the end of April!

There is huge hope among fans for this new era of the New England Patriots.

The alley off Boylston Street in Boston that was full of Emerson College student demonstrators for days now sits empty.

Many international students looking for jobs in Provincetown can't get cleared to work.

College students want their schools to divest from Israel. So how is tuition money linked to the war in Gaza?

Was the Drake Maye pick a HIT or a MISS? Are the Patriots WINNERS or LOSERS? Has the franchise found its QUARTERBACK OF THE FUTURE or are the Patriots DOOMED FOR ETERNITY?

"Messi Madness" is set to fully engulf Foxboro this weekend with a crowd of 65,000 expected to head to Gillette Stadium for their chance to see soccer royalty.

The Patriots got their quarterback in the first round of the 2024 NFL Draft on Thursday night, but New England's work is far from done this weekend.

Michael Hurley says the New England Patriots made the right pick with Drake Maye at number 3.

In his new role as an NFL Draft analyst, former Patriots head coach Bill Belichick wasted no time critiquing his old team's new quarterback, Drake Maye.