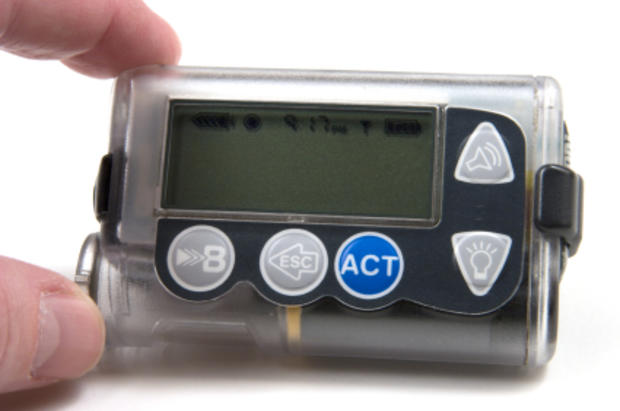
New Insulin Delivery Devices
Patients with diabetes now have a variety of methods from which to choose in order to deliver the insulin they need to manage their disease.
Without the right amount of insulin at the right time, patients can suffer a variety of serious problems and complications associated with their disease.
The conventional approach to delivering insulin is an injection using a syringe, which must be filled from a vial. But many patients are not thrilled with the method, often because they don't like needles or because it is hard to stay on a schedule of giving themselves frequent injections.
"It can be inconvenient," says Dr. Howard Wolpert, senior physician and director of the Insulin Pump Program at Joslin Diabetes Center in Boston, clinical partner of Beth Israel Deaconess Medical Center.
All patients with type 1 diabetes need insulin, as do many patients with type 2 diabetes who cannot control their blood sugar levels with medications. Some patients in this latter group are reluctant to begin injection therapy because of the psychological barriers.
Now, there are a growing number of alternatives to syringe/vial injections.
One popular alternative is the pen, which uses an insulin cartridge rather than a vial, as well as disposable needles. This method is much more popular in other parts of the world than in the U.S.
"It is much more convenient," says Dr. Wolpert. "It is still injected but the person doesn't draw from a vial."
However, the pen does have its drawbacks, according to Dr. Wolpert. These include higher cost and the fact that in cases where patients need mixed insulin they may need two injections.
Another alternative for many patients is the continuous subcutaneous insulin infusion pump, which is battery powered and delivers a continuous flow of insulin into a catheter. The pump is worn at all times but the catheter must be changed every few days.
When such pumps were first introduced, they were conspicuous because of their size, but are now much smaller. Plus, with so many people carrying cell phones on their belts, it is much less obvious when the device is a pump, since the pumps are about the size of a cell phone, he notes.
"The pump gives a more predictable dose from one meal to another," Dr. Wolpert says.
Pumps can be expensive but insurance usually covers them, especially for patients with type 1 diabetes.
So deciding between a pump and one of the injection methods is usually "a matter of personal preference," he says.
Other options include the injection port, which is similar to a pump but infuses the insulin through a port rather than a catheter. It requires fewer skin punctures than the traditional or pen method.
"There have been a lot of improvements over the past few years," he says. "But they have been mainly incremental improvements. I think pumps are the best way to go for people with type 1 diabetes. They can achieve tighter control with less risk of hypoglycemia. The pumps are much more accurate and precise."
About 35 percent of type 1 diabetes patients at Joslin use pumps, he noted.
Other ideas that have been tried or are being tried include inhalable insulin devices and trans-dermal patches, but neither has proven ready for prime time so far, he says.
One inhalable device was on the market but was withdrawn due to problems with lung toxicity, he says.
"They are still trying to develop it," Dr. Wolpert says.
Skin patches are also still under development.
"There have been several improvements in recent years and there are others in the works that should make it easier for patients to take insulin and improve insulin absorption," he says.
Above content provided by Beth Israel Deaconess Medical Center and clinical partner Joslin Diabetes Center. For advice about your medical care, consult your doctor.
Posted: November 2012